
Kevin Nicolin’s calling in life is to serve others. As the executive pastor at Henderson Hills Baptist Church in Edmond, Nicolin oversees the church staff and serves as an elder.
Four years ago, Nicolin began to experience tremors on the right side of his body. His family physician referred him to a neurologist, and he was diagnosed with Parkinson’s disease.
“In the beginning, it was a concern, but it wasn’t really pronounced,” Nicolin said.
Nicolin and Dr. Tyler Webb, a Mercy Clinic neurologist, began a long journey with medication to try to manage his symptoms. At first, he only needed the minimum dosage to control the tremors in his foot and hand, but eventually required two pills, four times a day.

“My days revolved around my pill-taking schedule,” Nicolin said. “Every day I had to strategize in four hour increments in order to balance meetings, eating, and when to take my medicine to function well."
He described the tremors as more than just an external shaking but also a disruptive, distracting feeling on the inside of his body. It affects everything he does, is aggravated by stress and makes it difficult for him to sleep.
“I used to be able to preach a few times a year and once the Parkinson’s hit, that ended,” Nicolin said. “It would be too distracting to me. I remember doing my mother-in-law’s funeral and it was extremely difficult for me to get through.”
He was referred to Dr. Cherian Karunapuzha, a neurologist at the Meinders Center for Movement Disorders at Mercy Hospital Oklahoma City, to talk about other options. Dr. Karunapuzha specializes in treating Parkinson’s disease and recommended deep brain stimulation (DBS), which involves implanting electrodes in the brain to help regulate abnormal body movements using electrical impulses.
“DBS essentially acts like a pacemaker for the brain,” said Dr. Karunapuzha.
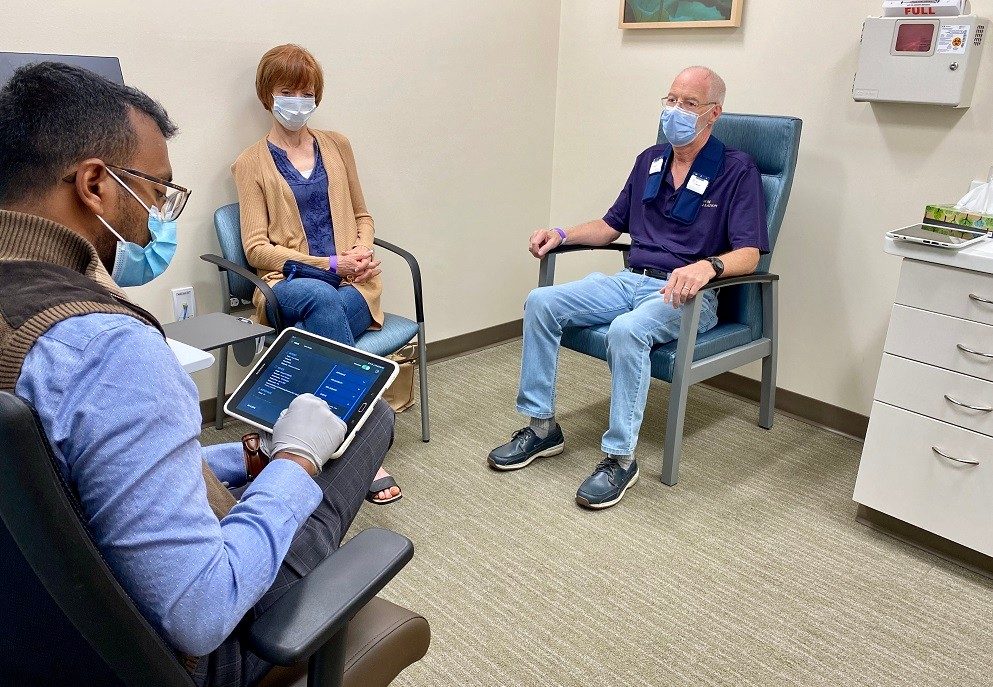
Mercy Hospital Oklahoma City has offered DBS for patients since 2018, but the FDA approved a new, upgraded version in June. The manufacturer, Medtronic, created a new battery, Percept, which continuously captures and records brain signals while delivering therapy to patients with neurologic disorders. Physicians can see exactly how the patient’s brain is responding to therapy via a program on a tablet and make adjustments in real time. Using this data, physicians can tell how much time in a day Parkinson’s patients spend feeling slow and stiff, mobile or experiencing excessive movements.
Previously, the only feedback during DBS came from patients describing their symptoms or how the electricity made the feel. With Percept, physicians can associate events in the brain with symptoms.
“This is a game changer because it shows us exactly how the brain is responding to the amount of electricity it is receiving,” Dr. Karunapuzha said. “We can use this new technology to more effectively help our patients reduce symptoms and have a better quality of life.”
Dr. Eric Friedman, neurosurgeon, placed the electrodes in Nicolin’s brain and implanted the battery during two different procedures in August.
After Nicolin recovered from those placements, Dr. Karunapuzha turned on Nicolin’s device in an outpatient office visit and adjusted the electricity to find a setting that made Nicolin feel most comfortable. During the visit, his tremors were visibly and significantly reduced. He has continued to improve and can now adjust the settings on his own.
“You’re always wondering, ‘Was this all worth it?’” Nicolin said. “So far, I really think this was worth it. I look forward to seeing how it helps me in the future because Parkinson’s is a progressive disease.”
Nicolin and his wife of 46 years have two adult children and four grandsons. His hope is that DBS will allow him to live a more normal life and make more memories with his family.
“The times when I feel normal – they are glorious, precious moments because they are so rare,” Nicolin said, “My hope and prayer is that I’ll continue to be able to work and play with my grandkids. Those are the things I really love to do.”

