
While COPD is a common lung disease, it’s just one of many that can be difficult to diagnose. That’s why a pulmonary function test can be beneficial.
Pulmonary function tests (PFTs) measure how well the lungs take in and exhale air and how efficiently they transfer oxygen into the blood. The tests measure lung volume and capacity, flow rates and gas exchange.
A pulmonary function testing can:
- Identify the high-risk smoker.
- Detect lung disease early.
- Determine the strength of breathing muscles.
- Evaluate the course of lung disease.
- Measure therapy effectiveness.
- Determine the cause of shortness of breath.
- Evaluate the effects of occupational exposures.
- Determine the degree of impairment.
- Evaluate the risk of complications after surgery.
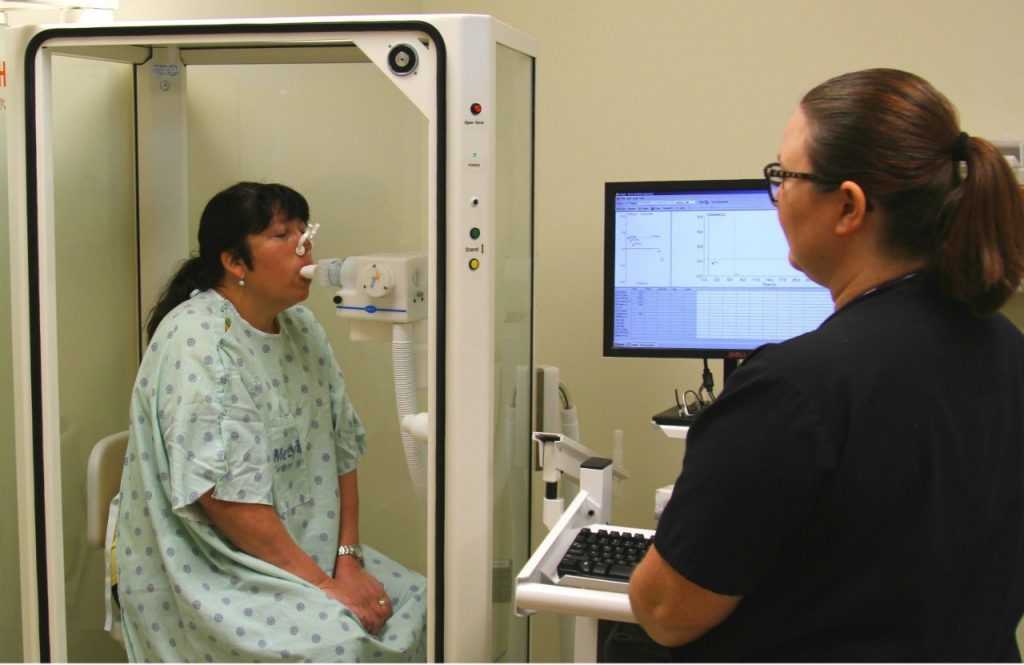
Many factors influence PFTs: weight, age, sex, race, environmental factors, altitude and, most importantly, a patient’s effort. Respiratory care practitioners like Sara Dobkins at Mercy Carthage have two methods to measure air moving in and out of the lungs:
- Spirometry, using a spirometer with a mouthpiece hooked up to a small electronic machine.
- Plethysmography, where the patient sits or stands inside an air-tight box that looks like a telephone booth.
“The plethysmograph measures residual volume, functional residual capacity and total lung capacity. It is the most accurate test for showing absolute volumes of air in the lungs, which helps the doctor diagnose any lung issues,” said Chalaine Bell, manager of cardiopulmonary services at Mercy Carthage and a respiratory care practitioner. “Pulmonary function tests can determine whether there is a restrictive problem, like a neuromuscular disease, or an obstructive problem, like COPD or asthma.”
The device is used for screening, diagnosis and trending after determining baseline settings.
“For patients with debilitating lung diseases, the doctor often will order PFTs every few months or yearly to monitor for any changes in pulmonary function and progression of their lung disease,” Bell said.
Some lung ailments can be difficult to diagnose, Bell said, so PFTs are vital to the process.
“A physician can look at lab work, X-rays and patient assessments. Those are all great tools,” she said, “but this gives you actual numbers so you know to what degree they are impaired or that, best-case scenario, they have normal lung function. It’s a great diagnostic tool, especially for pulmonologists.”
The procedure isn’t easy for respiratory care practitioners, who must calibrate the plethysmograph to room size, barometric pressure and temperature to ensure correct measurements, Dobkins said.
Although PFTs are not painful, they can be quite taxing for the patient, Dobkins said of testing that can take 30 minutes to an hour and involves varying lengths of time when patients breathe at differing volumes and intensities.
“It can be a difficult test and a lengthy test for those who have some type of health issue,” she said.
“The tests are very technique-dependent,” Bell said. “Patients have to understand that they need to give their best effort so we can give them the best results possible.”
For more information on cardiopulmonary services at Mercy Hospital Carthage on the McCune-Brooks Campus, call 417-359-1302.

