
It was 5 a.m. on a cold morning in February when Cris Gomes’ 4-year-old son climbed into bed and woke her up. Since she was awake, she decided to get up to nurse her 3-month-old baby. She picked him up out of his bassinet and propped him up on her right side. That’s when she knew something was wrong.
“All of a sudden I felt very tired all over my body, and I could not keep my eyes open,” said Gomes, a 35-year-old speech pathologist.
Gomes passed out and when she woke up, she didn’t know what happened. The baby was still in her arms and she was able to use her left arm to place him back in his bassinet. Her husband woke up around 6 a.m. and asked if she was OK. When she didn’t respond, he turned on the light.
“I took one look at her and knew right away she’d had a stroke,” Franciney Gomes said.
Cris Gomes couldn’t speak and the right side of her body was immobile. He called 911 and the ambulance rushed her to Mercy Hospital Oklahoma City, an Advanced Comprehensive Stroke Center certified by The Joint Commission. This special designation means the hospital has the most advanced imaging capabilities, 24/7 availability of specialized treatments and staff with the unique education and competencies to care for complex stroke patients.
EMS alerted the hospital’s stroke team and they were waiting for Gomes when she arrived.
“I’d just pulled into the parking garage when our stroke coordinator, Julie Bryant, called to tell me about this patient,” said Dr. Bahar Malakouti, neurohospitalist at Mercy Hospital Oklahoma City. “We were all very scared for her, and I went straight in to meet her for a CT scan.”
The CT scan showed there were no signs of brain bleeding, which meant she was a candidate for intravenous tissue plasminogen activator, or tPA, a powerful blood thinner that is the gold standard treatment for ischemic strokes.
“If you get to the hospital in time, we can give you this medication to help bust up the clot and restore blood flow to the affected part of your brain,” said Dr. Malakouti. “That’s why we say time is brain. It’s so important to get to the hospital as quickly as possible.”
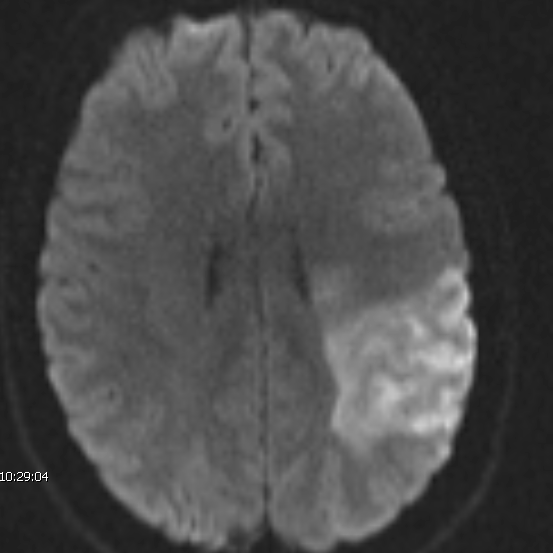
The imaging showed another concern – a large tear in the wall of a major artery and a clot in the area of her brain that controls her language, comprehension, and the motor control of the right side of her body. About 30 percent of arterial dissections are spontaneous, and Gomes didn’t have any known risk factors for the type of stroke she had.
Her prognosis was grim, and the stroke team sat down with her husband for a difficult conversation.
“I told him she may never speak again, she may never eat again, she may never be able to hold or nurse her baby again – all the things a new mom should be able to do. We truly did not think she would recover,” said Dr. Malakouti.
Dr. Bryan Van Zandt, an interventional radiologist, performed intraarterial thrombolysis, a procedure to dissolve the clot that was causing her stroke. While that procedure was successful, the team discovered another clot over the dissection in her artery that posed a dangerous risk to her brain.
“I had a very candid conversation with her husband,” said Dr. Van Zandt. “I told him we’ve done everything we can do. We’ve given her the best care possible, but we don’t know how things are going to turn out, so we just need to pray.”
Gomes was transferred to the intensive care unit, where she was closely monitored for 24 hours. A nurse checked her neurologic functions every 15 minutes.
“When I was in the ICU, I remember having a spiritual experience where I told God this was going to be too hard and it would be easier if I just died,” said Gomes. “How would I recover from this? I was ready to go and I was at peace with it. The only way I know how to describe it is I felt like I was going down, and God clearly said to me, ‘No, you’re going up.’”
The next day, Gomes had another CT scan.
“By some miracle, that second blood clot was gone,” Dr. Malakouti said. “We watched her slowly start to recover.”
She was walking with assistance the day after the stroke. On FaceTime with her family, she was able to say a few words and phrases like “yes,” “no” and “I love you.”
Before her stroke, Gomes worked as a speech pathologist in a skilled nursing facility, often with patients recovering from strokes.

“When I was in the hospital, the first time I worked with a speech therapist, I understood what was going on because of my work,” she said. “Even though I couldn’t really speak, I knew what was happening in my brain and I think that helped me.”
A few days later, she was discharged to Mercy Rehabilitation Hospital Oklahoma City, where she spent a couple weeks recovering. She spent hours every day working with physical, occupational and speech therapists. At that time, she couldn't hold a pencil or fork, so they worked on coordination and strengthening her right hand. Gomes struggled with aphasia, a speech disorder that affects her ability to speak and understand written and spoken language. In the early days of recovery, she couldn’t say the word “stroke.”
Four months later, she has made a near complete recovery.
“There’s no question she is a walking miracle,” said Dr. Van Zandt. “What our team did certainly played a role, but there’s so much more to her story than what we did.”
She’s driving again, able to care for her two boys on her own and participate in conversations.
“Speech pathologists that I know, my colleagues, most thought I would never speak again,” said Gomes. “The fact that it’s only been four months and I’m not only alive but I’m thriving, I think it’s a miracle.”
She continues to work with her Mercy outpatient speech language pathologist, Terri Bosnyak, twice a week. Bosnyak and Gomes often trade roles, allowing Gomes to practice doing patient evaluations as the speech therapist with Bosnyak as the patient. The goal is to get her back to work.
“There were things I read about and things I used with my patients that I now understand in a way that no one would be able to understand unless you’ve had a stroke,” said Gomes. “There’s textbook knowledge and there’s real life, and I know I’ll be able to relate to my future patients on a new level. They’ll have me as an example of what is possible.”
Signs & Symptoms of a Stroke
If you or a loved one is experiencing sypmtoms of a stroke, call 911 immediately. Brain damage can begin within minutes, and quick treatment can help increase the chances of a full and meaningful recovery.
An easy way to remember the signs and symptoms of stroke is to B.E.F.A.S.T.
B = Balance - Does the person complain of sudden onset unsteadiness, dizziness or difficulty walking?
E = Eyes - Does the person complain of narrowing vision, blurred vision, seeing dark or bright spots?
F = Face - Ask the person to smile & show their teeth. Is the smile even or lop-sided?
A = Arms - Ask the person to raise both arms and hold them straight out. Does one arm drift downward?
S = Speech - Ask the person to repeat a simple sentence. Do words sound slurred or garbled?
T = Time - Knowing the time when the person was last seen “normal” helps determine the course of treatment and improve outcomes.


